Knowing the basics of how to read a mammography report can put you at ease. If you’ve never seen a mammogram report before, it can be a little intimidating or confusing to try to understand the information it presents. Your doctor will also get a copy and may want to go over it with you, depending on your results. Once the mammogram findings are ready, you’ll receive a report. You might wait several days up to a few weeks, depending on the imaging center you use. (Having dense breasts also slightly raises your risk of getting breast cancer.)īI-RADS classifies breast density into 4 groups, which are described in Breast Density and Your Mammogram Report.Please find your nearest location on our locations page to call/schedule an MRI, CT, Ultrasound, or X-ray.Īfter your mammogram appointment, you likely won’t receive immediate results. The denser your breasts, the harder it can be to see abnormal areas on mammograms. Your mammogram report will also include an assessment of your breast density, which is a description of how much fibrous and glandular tissue is in your breasts, as compared to fatty tissue. Imaging may be used in this way to see how well the cancer is responding to treatment. This category is only used for findings on a mammogram (or ultrasound or MRI) that have already been shown to be cancer by a previous biopsy. Known biopsy-proven malignancy – Appropriate action should be taken The findings look like cancer and have a high chance (at least 95%) of being cancer. Highly suggestive of malignancy – Appropriate action should be taken For this reason, this category is often divided further:ĤA: Finding with a low likelihood of being cancer (more than 2% but no more than 10%)ĤB: Finding with a moderate likelihood of being cancer (more than 10% but no more than 50%)ĤC: Finding with a high likelihood of being cancer (more than 50% but less than 95%), but not as high as Category 5 The findings in this category can have a wide range of suspicion levels. The radiologist is concerned enough to recommend a biopsy. These findings do not definitely look like cancer but could be cancer. Suspicious abnormality – Biopsy should be considered This approach helps avoid unnecessary biopsies, but if the area does change over time, it still allows for early diagnosis. You will likely need follow-up with repeat imaging in 6 to 12 months and regularly after that until the finding is known to be stable (usually at least 2 years). But since it’s not proven to be benign, it’s helpful to be extra safe and see if the area in question does change over time. Probably benign finding – Follow-up in a short time frame is suggestedĪ finding in this category has a very low (no more than 2%) chance of being cancer. 
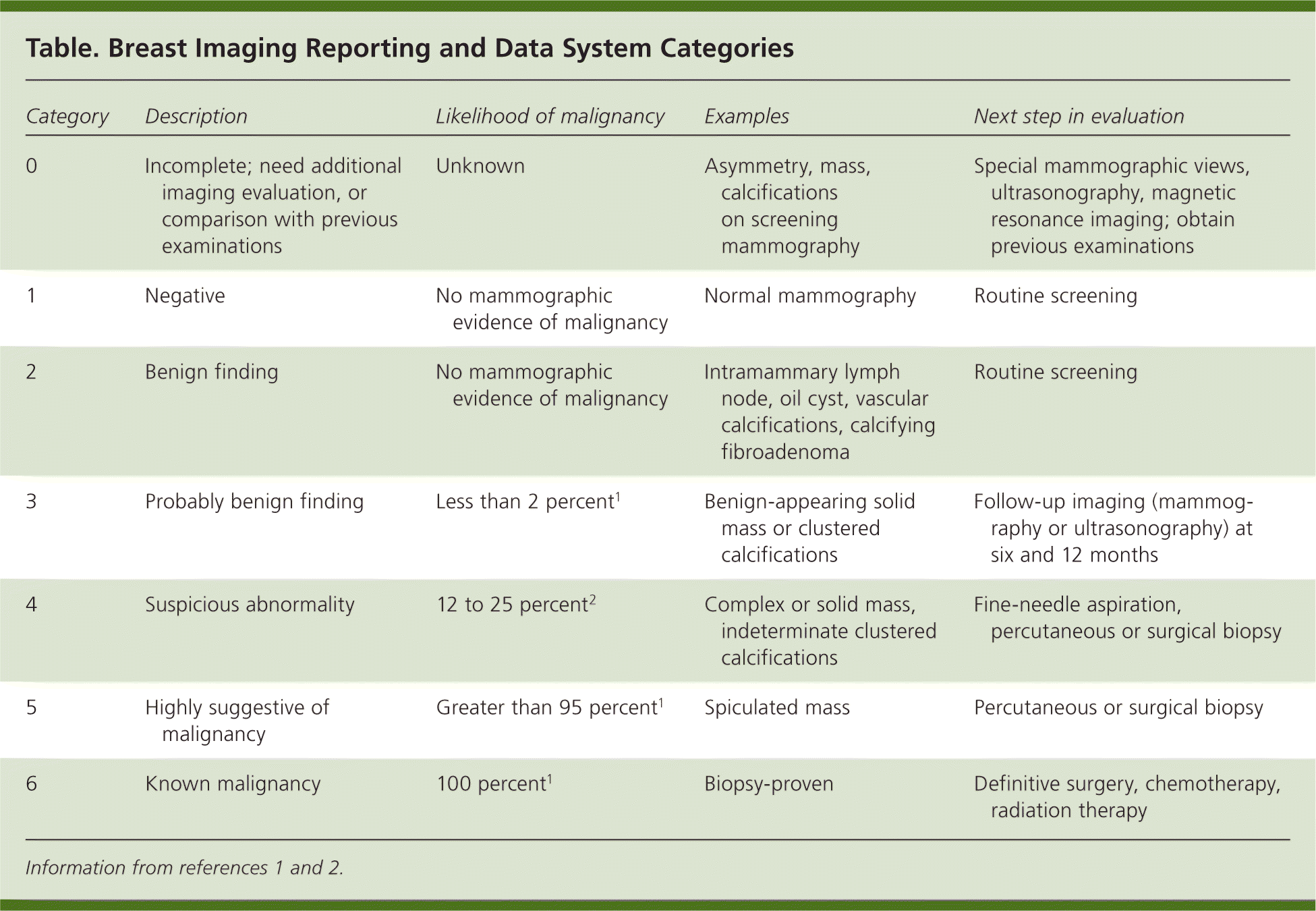
This ensures that others who look at the mammogram in the future will not misinterpret the benign finding as suspicious. This can also be used to describe changes from a prior procedure (such as a biopsy) in the breast. This is also a negative test result (there’s no sign of cancer), but the radiologist chooses to describe a finding that is not cancer, such as benign calcifications, masses, or lymph nodes in the breast. In this case, negative means nothing new or abnormal was found. Your breasts look the same (they are symmetrical) with no masses (lumps), distorted structures, or suspicious calcifications. This may also suggest that the radiologist wants to compare your new mammogram with older ones to see if there have been changes in the area over time. This means the radiologist may have seen a possible abnormality, but it was not clear and you will need more tests, such as another mammogram with the use of spot compression (applying compression to a smaller area when doing the mammogram), magnified views, special mammogram views, and/or ultrasound. Incomplete - Additional imaging evaluation and/or comparison to prior mammograms (or other imaging tests) is needed. However, the recommended next steps after these tests might be slightly different.) What do the BI-RADS categories mean? ( Note: These same BI-RADS categories can also be used to describe the results of a breast ultrasound or breast MRI exam. This makes communicating about the test results and following up after the tests easier. With these categories, doctors can describe what they find on a mammogram using the same words and terms. This system (called the Breast Imaging Reporting and Data System or BI-RADS) sorts the results into categories numbered 0 through 6. What is a BI-RADS assessment category?ĭoctors use a standard system to describe mammogram findings and results. Talk to your doctor about your mammogram results and what you need to do next. A doctor called a radiologist will categorize your mammogram results using a numbered system.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
